|
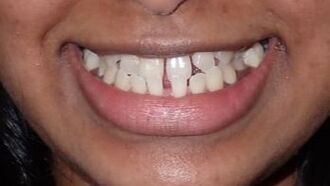
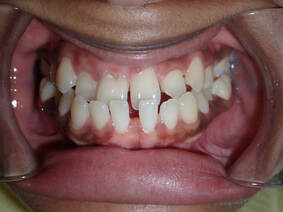
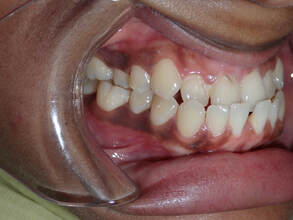
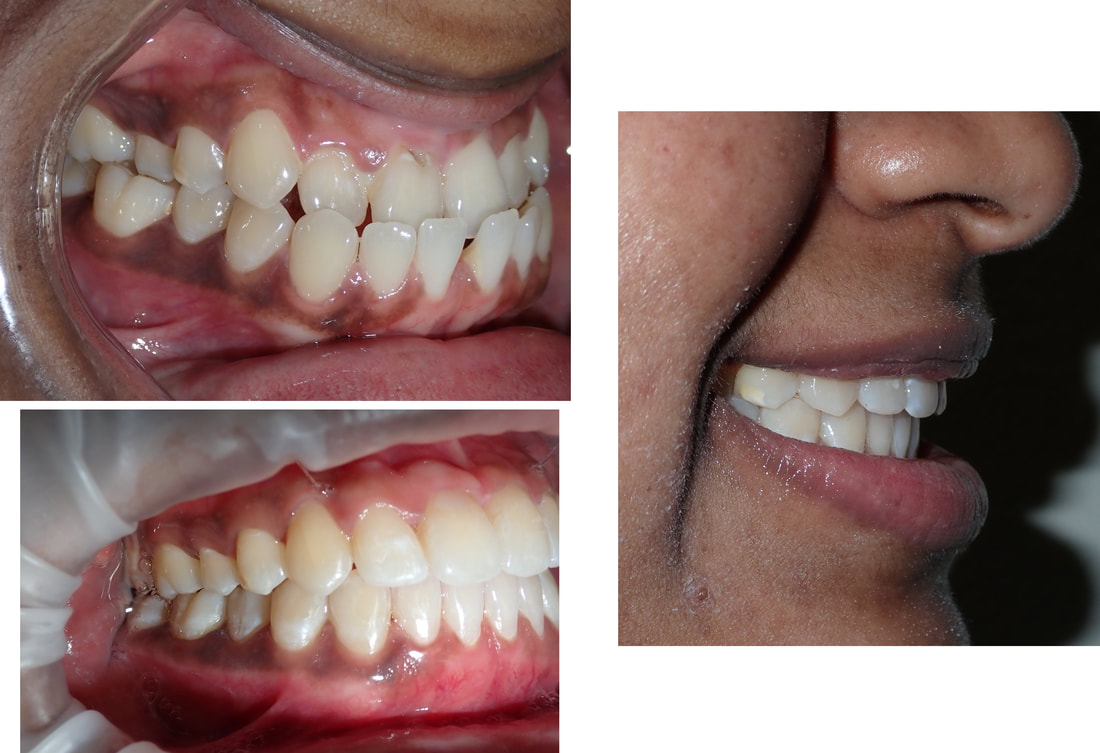
The magic of orthodontics! Many would see this case as beyond the scope of Invisalign. There's lots of spaces along with a severe deep underbite. However, we saw this as a fun challenge that could really change someone's life! As with all orthodontics cases, Invisalign success depends partially on the clinician, but MOSTLY on the patient. All patients undergoing Invisalign MUST: 1) Wear each aligner at least 20-22 hours per day - this allows the Invisalign aligner to maximize its time to move teeth 2) Only take the aligner off when eating, brushing and flossing. Otherwise it stays in the mouth at all times! 3) Make it to each and every single orthodontic appointment in the office 4) Don't lose the aligners! Make sure your pets stay away from these aligners, they think Invisalign is a chew toy :) We initially estimated this case would take about two years, based on the severity of the underbite and the amount of spaces to close between each tooth 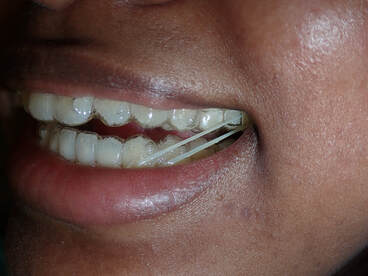 We use Class 3 Elastics (left) to help correct the underbite and re-position the mandible. Voila! This case took 14 months! Note the following changes:
1) Correction of the underbite to ideal overbite and overjet. 2) Closure of all the gaps between the teeth 3) Improved lip support and development 4) An absolutely stunning smile to show off!
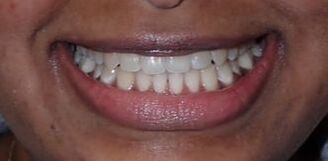
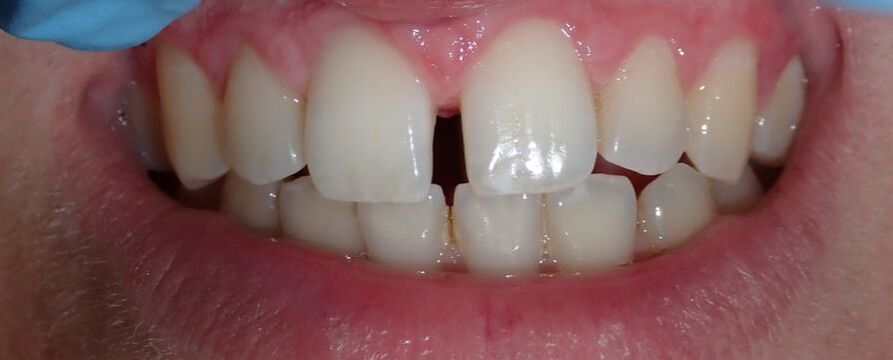
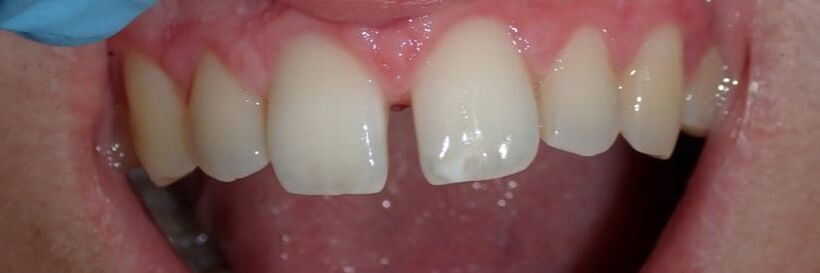
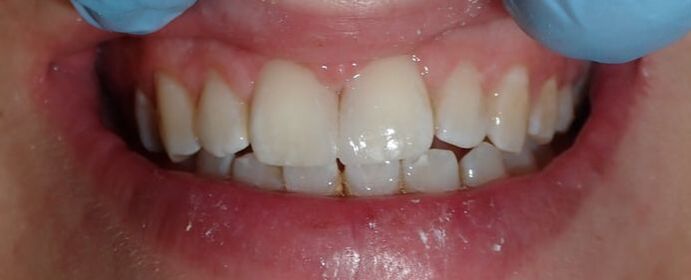
For many others, they wish to close their gapped teeth. Some common ways to do this are with 1) orthodontics like Invisalign, 2) with veneers and crowns, or 3) with a more conservative option - bonding. Orthodontics can be more costly and more time-consuming, veneers and crowns can be more costly and aggressive. Therefore, bonding fillings between the teeth remains the faster, more conservative, and cost-effective option. This teenage patient had been advised by mom and dad to get his front teeth closed with bonding. Some treatment plan considerations: 1) Orthodontics - he had done orthodontics before, but the teeth moved apart. There was a genetic component since his father had a similar gap between his teeth when he was growing up. He did not wish to do a second round of orthodontics since he had done it previously. 2) Veneers and crowns - this patient is a teenager, so drilling teeth would be my (and his) least desired option. 3) Let's do some aesthetic bonding! Using the Bioclear Matrix system (see previous blog post for more information), we were able to close his gapped teeth. We re-created a very natural appearance, with ideal shapes and curves, that is both esthetic and easily cleansible. These are the advantages of this matrix system!
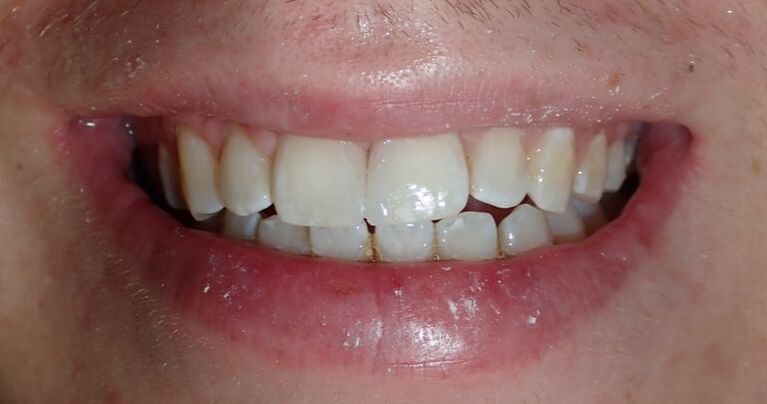
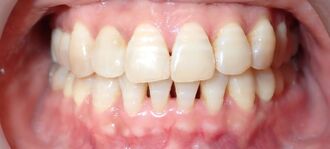
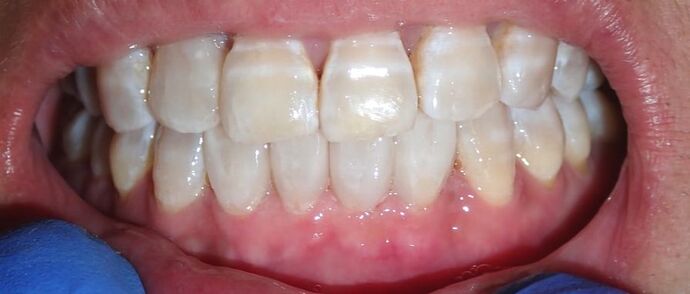
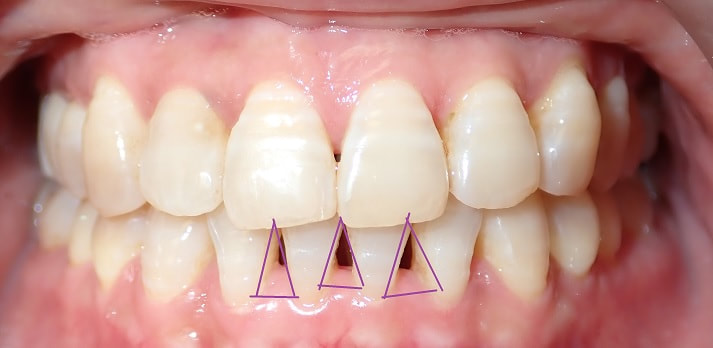
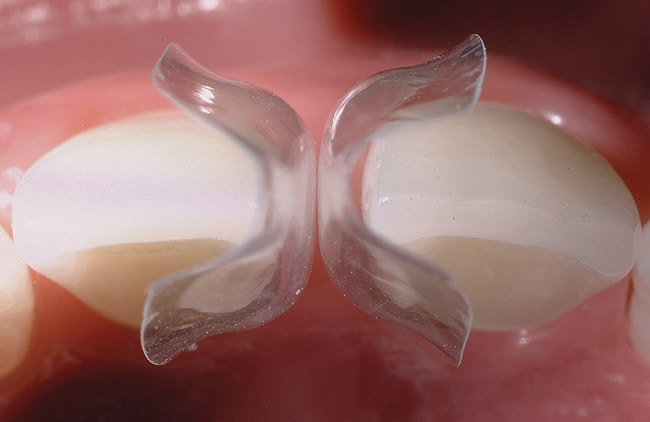
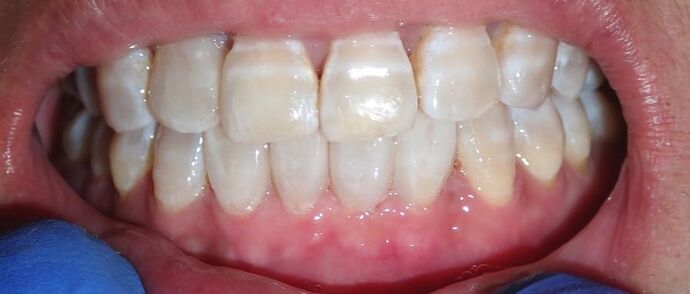
Black triangles occur when there is a loss of gum between the teeth. This can occur when there is a loss of bone due to disease, crooked teeth, or poor hygiene, among other reasons. These little "triangles" of "black" space (pictured below) tend to catch more food and plaque in the middle, along with being unaesthetic! When closing a black triangle space, we can't just stuff a filling in the middle and call it a day. Front teeth require specific anatomy and gentle curves not just for esthetics, but for ease of flossing and cleansing. The purpose of this anatomy makes it harder for plaque to catch in between and, thus, prevent bacterial growth which can lead to further gum loss. To remedy this, we place fillings between the teeth with a device called a Bioclear Matrix (below). This plastic Bioclear matrix template allows us to bond a filling that has all the right shapes and curves to give us an aesthetic AND cleansible restoration. Note how the unesthetic black triangle spaces are now filled with aesthetic restorations that have all the right shapes and sizes. The teeth and gums are easily cleansible and will significantly reduce the amount of plaque trapping between the teeth. This patient's smile now looks many years younger!
|
AuthorDr. Mat and Dr. Jen will occasionally post cases or pictures from our office! Archives
August 2023
Categories |
Photo from Michael Dunn~!